Patient perspectives on surgery.
Sign up for new patient stories and practical resources straight to your inbox.

The woman who wouldn't take no for an answer: Natasha’s story
When doctors told her surgery was off the table for her stage 4 EGFR lung cancer, Natasha Loveridge went to the scientific literature. What she found may help change how stage 4 lung cancer is treated in the UK.

I believed I was a candidate for surgery. I began by asking my team if we could talk about it.

Natasha Loveridge is a teacher and a mother from Leeds in the UK. She used to run three times a week and followed a mostly vegetarian diet. She had no reason to read oncology journals or question national treatment guidelines — or to imagine she might one day need to.
That changed in December 2022 when she received lung cancer diagnosis at age 48. What followed was a shift in both stage and outlook, as her disease progressed to stage 4 in the early months of treatment.
In the precise vocabulary of oncology, Natasha is an EGFR-positive stage 4 lung cancer patient with a history of brain metastases. She is also someone who sits at a kitchen table late at night, reading clinical papers written for specialists, and sending emails to oncologists with subject lines like: I believe I am a candidate. Can we talk about this?
It was this instinct — to research, to question, to ask what else might be possible — that led her beyond the limits she had first been given, and into a part of the system that is not often visible to patients at all.

A diagnosis, and a door closing
The message from Natasha’s clinical team was delivered with kindness but without ambiguity: the cancer is incurable, and surgery was not an option. The focus would be systemic treatment.
Because her cancer carried an EGFR mutation, she was eligible for a targeted therapy rather than standard chemotherapy. She was started on osimertinib — an oral medication designed to inhibit the specific genetic driver of her tumour.
It worked. Her primary tumour shrank from 8.5 cm to 2.5. Brain metastases that had been visible on imaging appeared, for a time, to resolve.
She was doing well. And yet she understood, because her team had been honest with her, that she was living on borrowed time of a particular kind. Resistance to drugs like osimertinib is not a possibility; it is an inevitability. The question is always what comes next. For most stage 4 lung cancer patients in the UK, the answer does not include surgery.

The gap in the guidelines
In the UK, national guidelines do not set out a clear role for surgery in stage 4 lung cancer. In practice, this absence of guidance means the option is rarely raised and often quickly dismissed. The prevailing clinical approach is that operating on a primary tumour when disease has already spread is unlikely to offer meaningful benefit alongside significant risk.
Professional bodies, including The Society of Thoracic Surgeons and the European Society for Medical Oncology, have begun to reflect this nuance. In the UK, that nuance has yet to translate into formal guidance. And in the absence of guidance, the conversation is often absent too.
Natasha wanted to question this UK convention.

The research, the emails, the second opinions
Natasha began to suspect she might qualify under this emerging category. She read the literature, found case reports from the United States, and contacted patients in other countries who had undergone similar procedures. Then she brought it to her clinical team — not as a demand, but as a question backed by evidence.
Her clinical team listened. They also described her as an exceptional candidate. They sought opinions from the Royal Marsden and Royal Brompton, and from specialists in the US and Europe. The response, eventually, was a cautious yes.
Cases like this remain uncommon, and not part of a standard pathway — often dependent on a patient raising the possibility in the first place. As Natasha puts it herself, someone had to push. She did.

It was a tricky surgery and recovery. That’s why it’s important to understand all the risks.
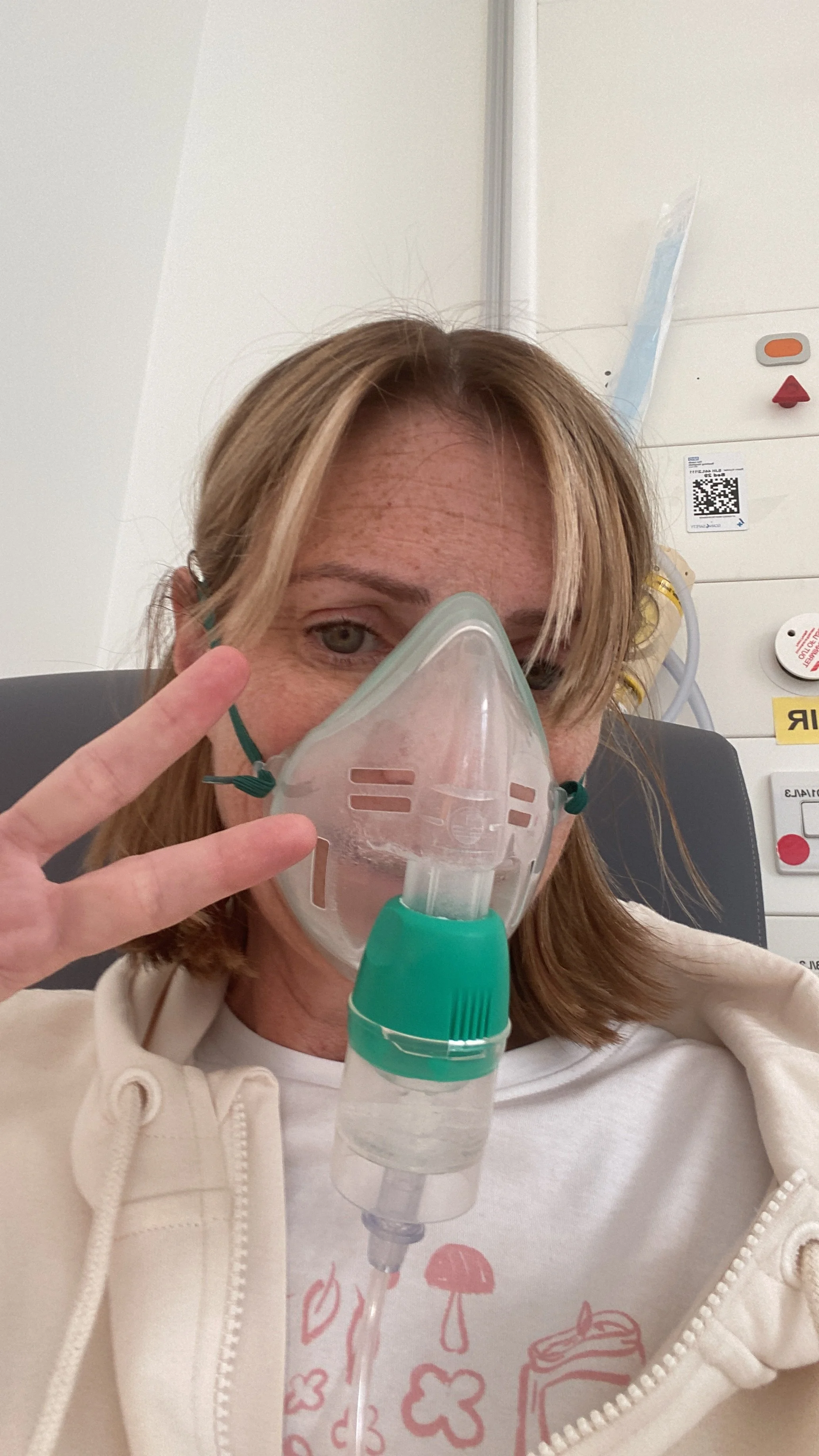
What could not be seen in advance
The surgery, when it came, was complex and did not end with the operation alone. Osimertinib — the targeted therapy that had kept Natasha’s disease in check for nearly three years — had altered her lung tissue, making it fragile and adhesive and complicating the procedure.
“It was a tricky surgery and recovery,” she says. “My targeted therapy made the tissue more complicated. This is why it’s important to have understand all the risks in your conversations with your team, and to build the trust for them to handle the unexpected.”
Surgeons removed the top right lobe of her lung as planned. However, because of the adhesions, they were unable to achieve clear margins — meaning not all cancerous cells could be removed with a clean boundary. As a result, Natasha also underwent 15 rounds of radiotherapy to her chest and trachea to consolidate any remaining disease.
In situations like this, the full extent of what surgery will involve — and what it will ultimately achieve — cannot be known in advance. Plans are made carefully, but they are also shaped in real time by what is found once surgery begins.
Natasha describes her outlook as clear-eyed but hopeful. “I feel I am receiving the best possible care,” she says. “And I’m grateful to my team for having the courage to follow the protocol of the North Star Trial.

Paving the way for different conversations
This is not a cure, and Natasha has never framed it as one. Stage 4 lung cancer remains an incurable diagnosis.
Natasha describes her goal simply. “It is my dream to hear the words ‘no evidence of disease,’” she says. “And I hope the local consolidation therapy will eventually make this dream a reality.”
That sense of possibility sits alongside a wider shift in how some lung cancers are understood. Many people with oncogene-driven disease are younger, fitter, and able to tolerate more intensive treatment than the traditional profile of lung cancer patients once suggested.
Natasha is now 52, and her two daughters are at that in-between stage — no longer small children, but still very much at the beginning of adulthood and everything that lies ahead. What surgery of this kind may offer is time: time to be present for those years, and time for the possibility that treatment will continue to evolve alongside the disease. It’s also why Natasha believes that access to those possibilities should not depend on a patient knowing to ask.
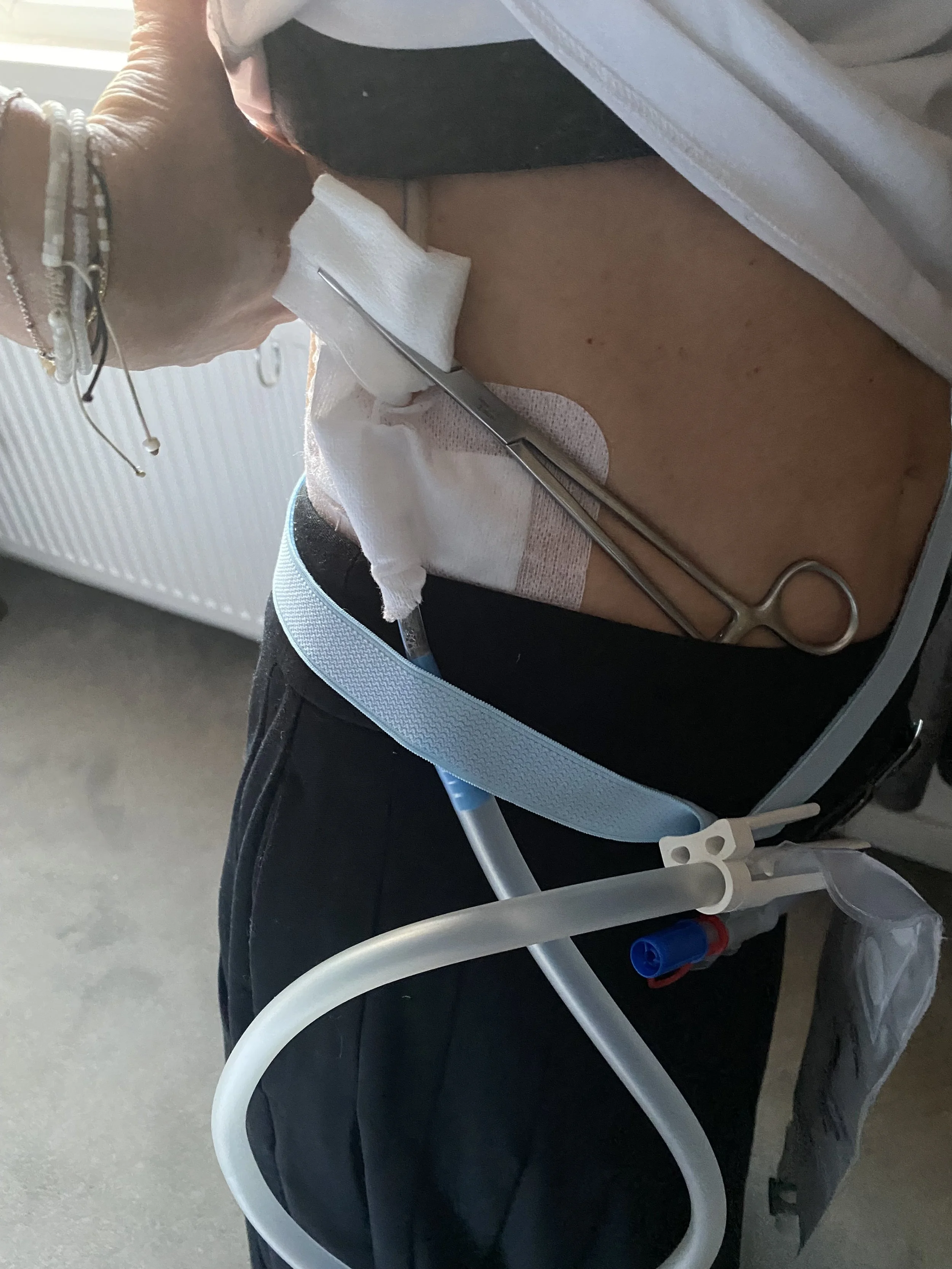
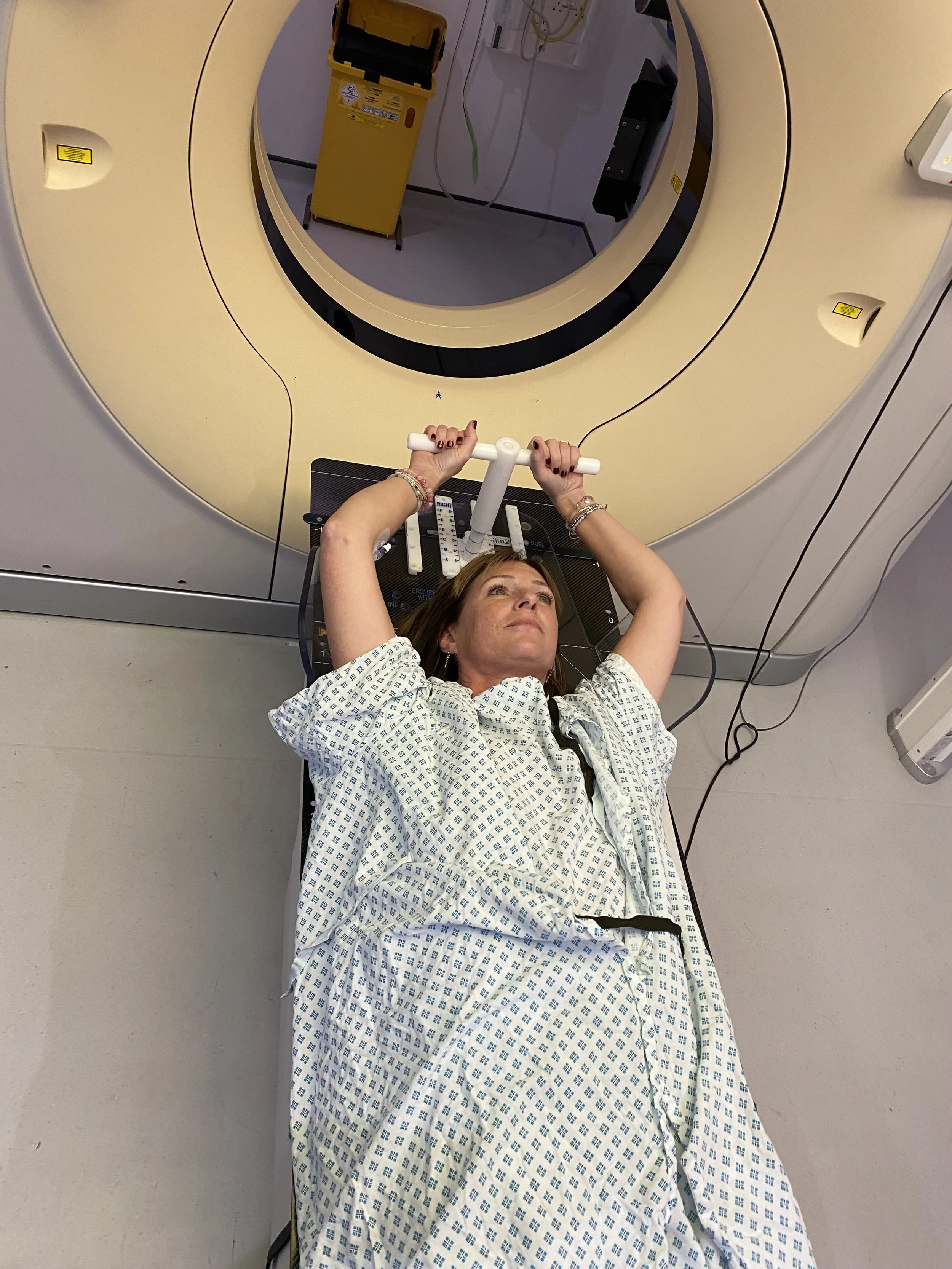

May 2026
