Patient stories.
Get real stories of people living with lung cancer.


If I had been diagnosed even a year earlier, perhaps it would have been stage 1 or 2.
— Nichol (R), initially diagnosed with stage 3A non-small cell lung cancer with no biomarkers at age 48. in 2018
Meet Nichol.
Nichol’s persistent cough was dismissed for years. By the time doctors looked again, the cancer had already been there for five years.

I honestly was the healthiest I’d ever been. There was no way it was supposed to be something serious.

Nichol had been coughing for years. Not the alarming kind, just a stubborn cough that followed every cold and refused to leave. It interrupted meetings, woke her at night, then faded into the background of daily life.
Living in London since 2005, fit, healthy and exercising regularly, she was the picture of health.
Yet the cough persisted.
"I'd get sick and then the cough would just stay for weeks and weeks," Nichol recalls. She went to her GP. Again. And again. By 2015, they finally sent her for x-rays. The results, she was told, showed nothing.

When persistence turned to desperation
By 2018, something had shifted. The cough was worse. The exhaustion had also become overwhelming – making it a struggle to get through the workday. Her coughing fits were so severe she'd have to leave meetings.
The cough became background noise – yet it began interrupting everything from meals to movies. In desperation, Nichol’s husband suggested she use a counting clicker.
2,000 times a day.
Finally, enough was enough. Tiring of years of trying to "learn to live with it," Nichol walked into her GP's office and stopped being polite.
“I basically said I just can't live like this anymore. It's disrupting my life. I can't sit in a meeting without getting up and leaving the room. I cough to the point of incontinence. It's all embarrassing."
It was only when she stopped being a good patient — stopped downplaying, stopped being understanding about the system's limitations — that she was heard.
They sent her for another chest x-ray. The radiographer initially refused: "We've already taken this x-ray. We don't do the same x-ray twice." Again, she refused to take no for an answer.
As Nichol left the appointment, she didn't get 30 feet away before the radiographer called her back.
"There's a shadow." He tried to reassure her, but he said he wanted to be sure. Within hours, she was sent for an MRI. The next morning, she walked into a consultation room with a doctor with the extra support of a nurse – that telltale sign – when she was told she had advanced lung cancer. She was only 48.
"I honestly probably was the healthiest I'd ever been," she says, the disbelief still evident years later. "There was no way it was supposed to be something serious."
The shadow that was always there
Her pulmonologist went back and looked at her x-rays all the way back to 2015.
He found that the cancer had been visible on her scans for five years—the same scans they'd told her showed "nothing."
"If I had been diagnosed even a year earlier, perhaps it would have been stage 1 or 2," Nichol shares.
The primary tumour sat in the lower right lobe of her lung, with lymph nodes involved — one close to the heart, another further up. The staging came back as 3A. It was serious but still considered potentially curable.
There was no time to think. It was a Friday when she was told. That afternoon she phoned her family. By Monday she was gowned up in an operating theatre ready for surgery.
Nichol’s resected tissue was sent for full biomarker testing — the modern compass meant to guide lung cancer care. Doctors searched for EGFR, ALK, ROS1 and the growing list of mutations that can open doors to targeted therapies. Nothing actionable was found.
Without a driver mutation, the plan was the standard curative route: four rounds of chemotherapy — starting with cisplatin, then switched to carboplatin after she developed tinnitus and neuropathy — combined with 30 rounds of radical radiotherapy.
The chemo hit her harder than she could have imagined.
“The nausea and dizziness were unreal — even with anti-sickness meds. I didn’t feel part of the world. I felt like I was in the upside down from Stranger Things and I was the only one who could see it. I was on so many pills — if it wasn’t for my husband, I don’t know what would have happened.”
He became her anchor, managing medications, making her eat and drink, taking her outside each day. After the second cycle she tried to walk alone and collapsed in Muswell Hill. “Two women saw me go down and called an ambulance.”
Radiotherapy was gentler but relentless: six weeks of daily treatments, the machine buzzing as green lasers circled her body.
“I remember thinking, what the hell has happened? This isn’t real.”
Through it all, Nichol held to one thought: getting back to normal life.

Trying to live in the “after”
When treatment ended on 14 June, 2019, surveillance began over a six-year period. Scans every three months. Then every six. Eventually, once a year.
“I just wanted to survive this and close the door. I didn’t want cancer to become my identity,” Nichol shares. She did not join any patient groups. She avoided cancer conversations as she worked to keep cancer quiet in the background.
Friends reacted in ways she never expected. Some stayed close. Others vanished. So, she built a different life: back to exercise, back to work, back to everyday activities.
“I had people I considered really good friends just disappear,” she says.
By year six, her oncologist allowed himself a near-forbidden sentence. He said he didn’t like to use the word cured — but six years was a significant milestone. Her bloods were good. Her chest scan was clear.
She walked out of that appointment believing the worst was behind her.

Six years of borrowed breath
But around that time, in March 2025, she also began having headaches.
They were at the back of her head, sometimes accompanied by flashes of spiky rainbow lights across her vision. She blamed new glasses, tension, anything she could think of. At her annual oncology appointment, she mentioned them almost casually.
Her oncologist wasn’t worried. The scans looked great. He suggested physiotherapy, an eye test, a visit to the GP.
When Nichol’s GP insisted on a brain MRI because of her history, she felt more irritated than afraid.
“I remember thinking, lung cancer is never going to leave me,” she says. “It’s always going to be ruining my life.”
The scan was on a Friday. That evening, her phone rang.


There are tumours in your brain.
The phone call no one prepares you for
She heard her much adored oncologist’s voice and felt relief.
“Isn’t he kind – he’s calling so I don’t worry all weekend,” she thought.
Then he said, “There are three tumours in your brain.”
“I don’t know what happened after that,” Nichol says. “I ended up on the floor in the hallway. I handed the phone to my husband because I couldn’t hear anymore.”
“I kept saying out loud, ‘It’s going to kill me.’”
Choosing between impossible options
Within days Nichol was seeing neurosurgeons and radiotherapists. The largest tumour lay at the back of her head, in an area that controls vision. Nichol was keen on surgery — but it would come at a cost.
“I was told would likely lose depth perception and peripheral vision, perhaps the ability to drive, maybe even aspects of my work.”
What completely changed her mind was time. One surgeon explained that even a small complication from surgery could delay follow-up treatment, and any delay might be too late.
“That sealed it,” she says.
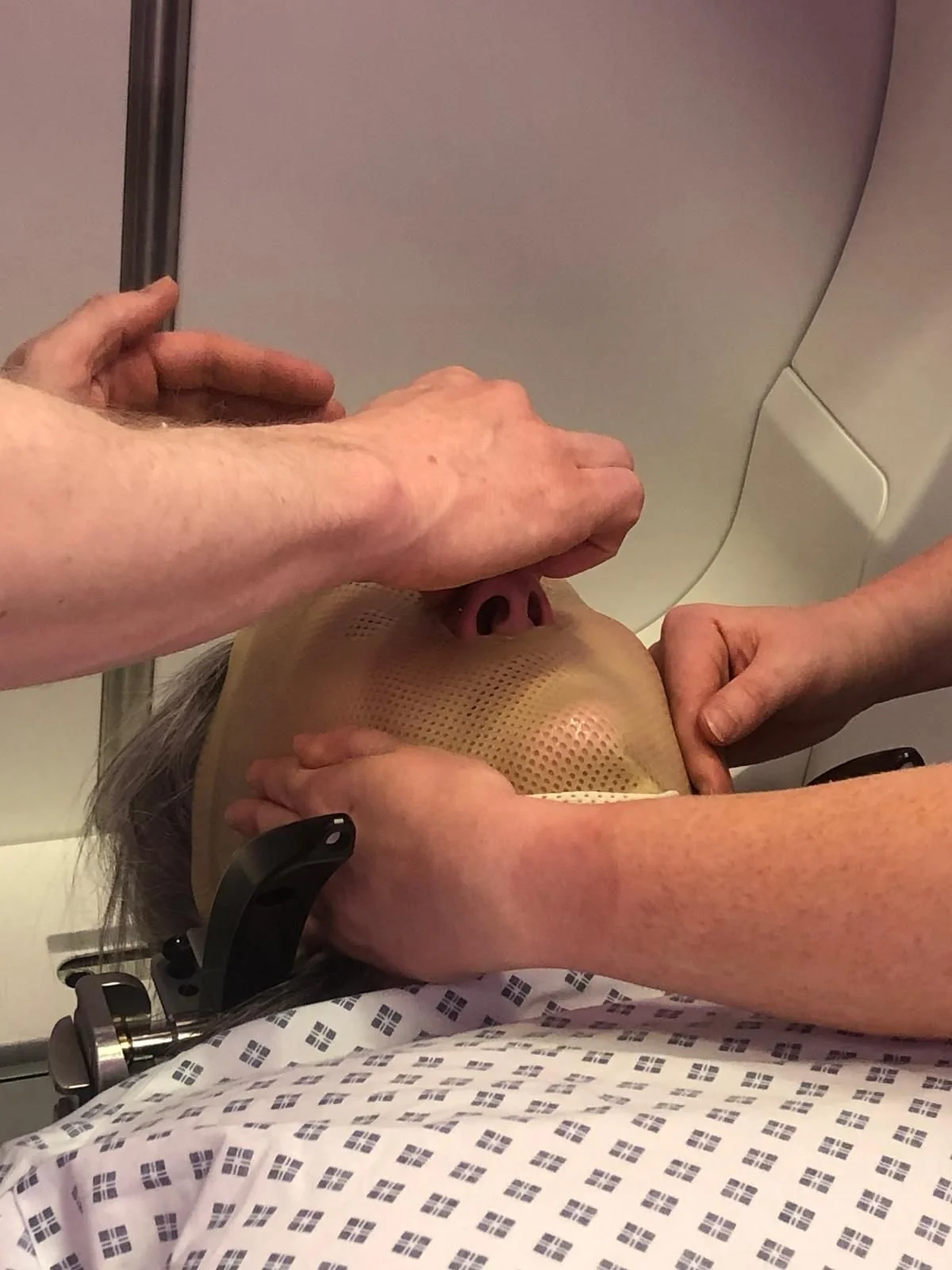
In April 2025 she underwent three sessions of Gamma Knife radiotherapy, her head fixed in a moulded mask while targeted beams treated the tumours. Doctors searched again for a biomarker through a lumbar puncture. A low HER2 signal was noted, but not enough to guide treatment.
“It’s strange to be disappointed not to have a mutation,” she says, “In lung cancer those letters can mean hope.”
In June she restarted chemotherapy: four cycles of carboplatin and pemetrexed, followed by pemetrexed maintenance every three weeks — later stretched to four to manage side effects. By then her veins had given up after years of needles, so treatment moved to a port.
That summer was brutal.
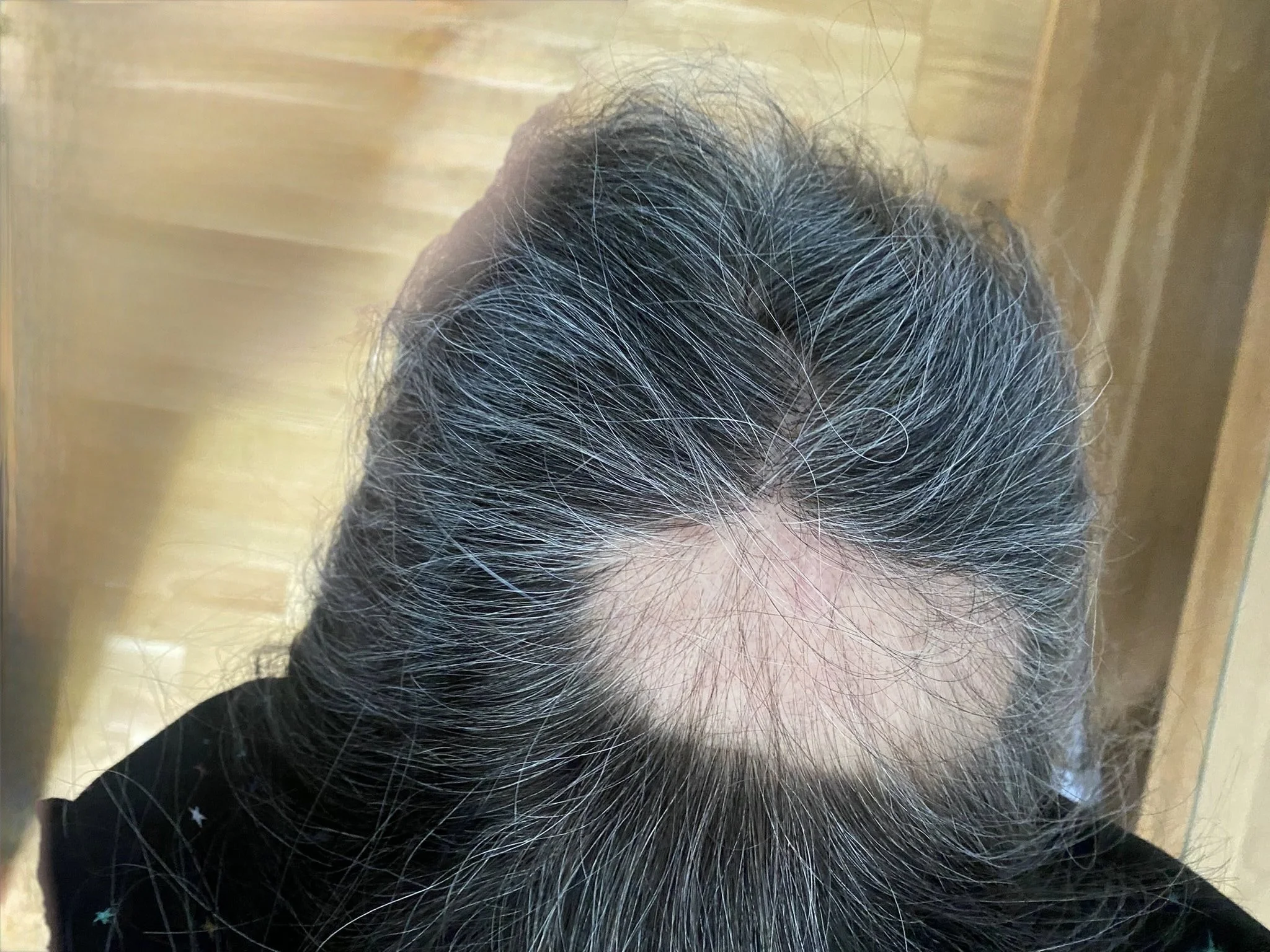
The hair changes came first. Gamma Knife left a small bald patch at the back of her head — a neat, circular mark she tried to hide with clever partings. Then chemo thinned the rest by about 50% but that has now settled.
The platinum fatigue and nausea returned, but the drugs also upended hormones already fragile from her first chemo-induced menopause. During a heatwave she was soaked with hot flashes, sweating through clothes despite HRT. Blood tests showed almost no oestrogen or testosterone. Her dosage was increased, and slowly the storm eased.
“It was a very, very rough summer,” she says.

Living with the word again
Today Nichol is in the strange space called “no evidence of active disease.”
The tumours responded. For now, there is stability. But treatment continues.
The lung cancer progression has changed the colour of everything for Nichol.
“It’s impossible to put it behind you,” she says. “It’s still in the peripheral vision, staining everything I look at.”
She has begun to reconsider the distance she once kept from other patients. There are events she wants to attend, people she hopes to meet. “I think I missed out by staying away from the patient community,” she shares. “I didn’t understand how much it helps to talk to people who get it.”

Still here, still her
Today, Nichol lives with stage 4 lung cancer — a life measured by scans, infusion chairs, and a calendar that’s never fully hers. She offers simple, hard-won advice.
“Don’t do it alone. I thought I had to be strong by keeping it all to myself,” she says. “And I wasn’t taken seriously by my GP until I came in angry and refused to accept no. Don’t worry about being polite.”
She wants her story to reach others like her: young, no biomarker. “It can feel like you don’t belong anywhere, like everyone else has a map and you don’t. You’re not alone.”
Nichol’s life is smaller in some ways, larger in others — measured in hospital corridors, yes, but also in the simple pleasures. There are still plans to make, mornings to wake up to, and that, she says, is everything.
February 2026
