Patient stories.
Get real stories of people living with lung cancer.
Meet Loryn.
When 34-year-old Loryn felt her body failing, doctors said it was stress, pneumonia, even possible rheumatoid arthritis. Six months later, she learned it was stage four lung cancer.

My husband would say, 'This isn't the woman I married. This isn't you. There's something going on here.’


Loryn knew something was wrong.
It was July 2023, a scorching day in Western Massachusetts. She was at a park with her three-year-old son, running around the playground like any young mom would. Except she couldn't breathe.
Sharp chest pain cut through her. She was winded—far more than she should have been. And that persistent back pain near her shoulder blade? It had been there for weeks now, gnawing at her.
"This isn't right," she told her husband. "Take our son home. I'm going to the ER."
It was her third emergency room visit in six months. She'd been hiking and camping with her family just months before, full of energy, planning to grow their family. Then, after her gallbladder removal, everything changed. The fatigue crept in. Her doctors kept telling her the same thing: Every young mom feels this way.
They prescribed antidepressants. Anti-anxiety medication. Anything but answers.
"My husband would say, 'This isn't the woman I married. This isn't you. There's something going on here,'" Loryn recalls.
She was right to be worried. But it would take six more months—and three more ER visits—before anyone believed her.
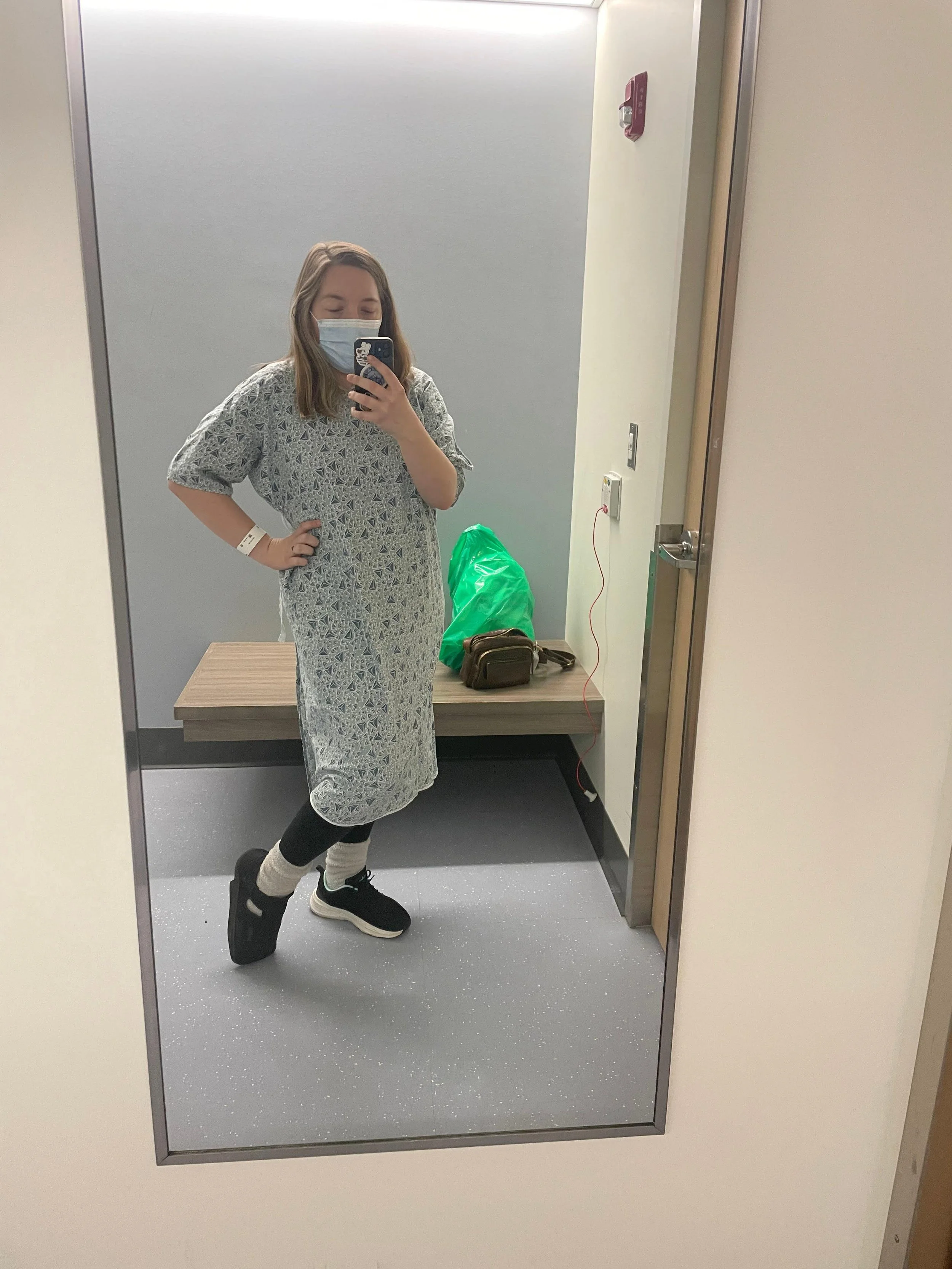
The nightmare of being dismissed
The first emergency room scan showed "very small ground glass nodules" in her lungs. Pneumonia, they said. Here's some antibiotics. You'll be fine.
A week and a half later, the antibiotics hadn't worked. The back pain persisted. She went back to the ER. Another scan. Same diagnosis: probably just pneumonia. But this time, something in the doctor's voice changed. "It's not behaving the way we'd expect pneumonia to," he admitted.
He referred her to a pulmonologist – miraculously getting her an appointment within a week at a clinic that was otherwise booking a year out.
The pulmonologist looked at her scans and saw a young, healthy woman. "I don't see anything concerning," he told her. "I don't want to put you through a bronchoscopy for something that could be nothing." He suspected an autoimmune condition and sent her to a rheumatologist.
But the rheumatology appointment was four months away.
During those months of waiting, new symptoms erupted. Excruciating joint pain – her knees, ankles, feet, hips. Sharp enough to make her think it was rheumatoid arthritis. The pulmonologist agreed: "Just wait for the rheumatologist."
Then one weekend, she developed a cough. She coughed so hard she felt a sharp pop in her ribs.
"Great," she thought. "Now I think I’ve broken a rib from coughing."
She went back to the ER. Her husband was exasperated: "You've had so many scans. We've got to figure out something."
But Loryn knew. Deep down, she knew something was terribly wrong.

"You've got lesions to your ribs, your spine, your liver"
The ER doctor brushed her off at first. "I think you'd know if you broke a rib," he said dismissively. "I don't think you'd break a rib from coughing."
But Loryn insisted. She wanted the scan.
When he came back into the room, his face was white as a ghost.
"I hate to tell you this," he said slowly, "but you've got lesions to your ribs, your spine, your liver. I see a large nodule in your lungs. You need to be checked out for metastatic disease."
Loryn was alone. Her husband was home with their son – it was just supposed to be a broken rib check. She texted him frantically while nurses prepared to transfer her to a larger hospital. By the time she was admitted, she was crying to a nurse, the weight of months of dismissal and fear finally breaking through.
Loryn spent a week in the hospital waiting for a biopsy. They other option was going back hoping and waiting a month for the appointment. She stayed.

Even then, she didn't think it was lung cancer. The nodule was so small. Loryn had taken such good care of her lungs. After having childhood asthma, she avoided smoke and any triggers religiously. Lung cancer felt impossible.
Then came the phone call.
Someone from the cancer department called while her husband was at work, her son at school. Casual. Matter-of-fact.
"I'm just calling to let you know that the results of your biopsy have come back. It confirms that you have stage four lung cancer."
Loryn was stunned into silence.
"I tried to ask questions," she remembers, "and they said they couldn’t answer anything right now. I was told they would talk to me at my oncology appointment in four weeks.'"
Four weeks.

The breakdown and the breakthrough
Loryn called her husband and told him to come home. Then she had what she describes as a full panic attack.
She could barely walk at that point – the lesions in her legs and knees were so painful. She imagined herself deteriorating from here, losing everything, leaving her four-year-old son without a mother.
"This is it," she thought. "I'm going to lose everything.
Her husband's brother, a psychiatrist at Mass General Hospital, immediately said: "You're not staying at that hospital. You're coming to Mass General."
They got her in within two days. Not four weeks.
Her new oncologist was different right from the start. She spent time educating Loryn about non-small cell lung cancer, about biomarkers and what she should expect. She explained that Loryn would likely have a biomarker – she was young, with no history of smoking – she fit the profile.

"She walked me through what could happen from here," Loryn says. "What it would look like if I didn't have a biomarker. She was really great about educating me, so that I didn't go to Google."
The blood test came back a week later: HER2-positive. Loryn's first reaction was disappointment.
"I had this strange hope," she admits. "I was secretly hoping for EGFR or one of the more common mutations that I'd read had many treatment options. HER2 was only 1% of lung cancers. I thought that of course I've got this super rare biomarker they don't know a lot about."
But her oncologist saw it differently. Her oncologist’s focus was on HER2 lung cancer. She was optimistic – realistic – but optimistic.
"There are a lot of treatment options out there," she told Loryn. "A lot of clinical trials. There's hope."

From crutches to swimming
When Loryn started treatment in late 2024, she was walking with a cane. Sometimes crutches. She couldn't bear weight on her left leg. Lesions had spread to every major bone and joint in her body – her elbows, knees, feet, the top of her skull, her jaw.
She began palliative radiation just to help her walk again. Then chemotherapy: carboplatin and pemetrexed.
"I told my husband that we needed to find a wheelchair. I feared I was going to end up in a wheelchair from this. I just felt that there was no way this was going to get better.'"
But it did.
Just not right away. Unfortunately, after just over two months, Loryn’s cancer progressed on the first-line chemotherapy. Her oncologist had hoped for six months. Two months felt devastating.
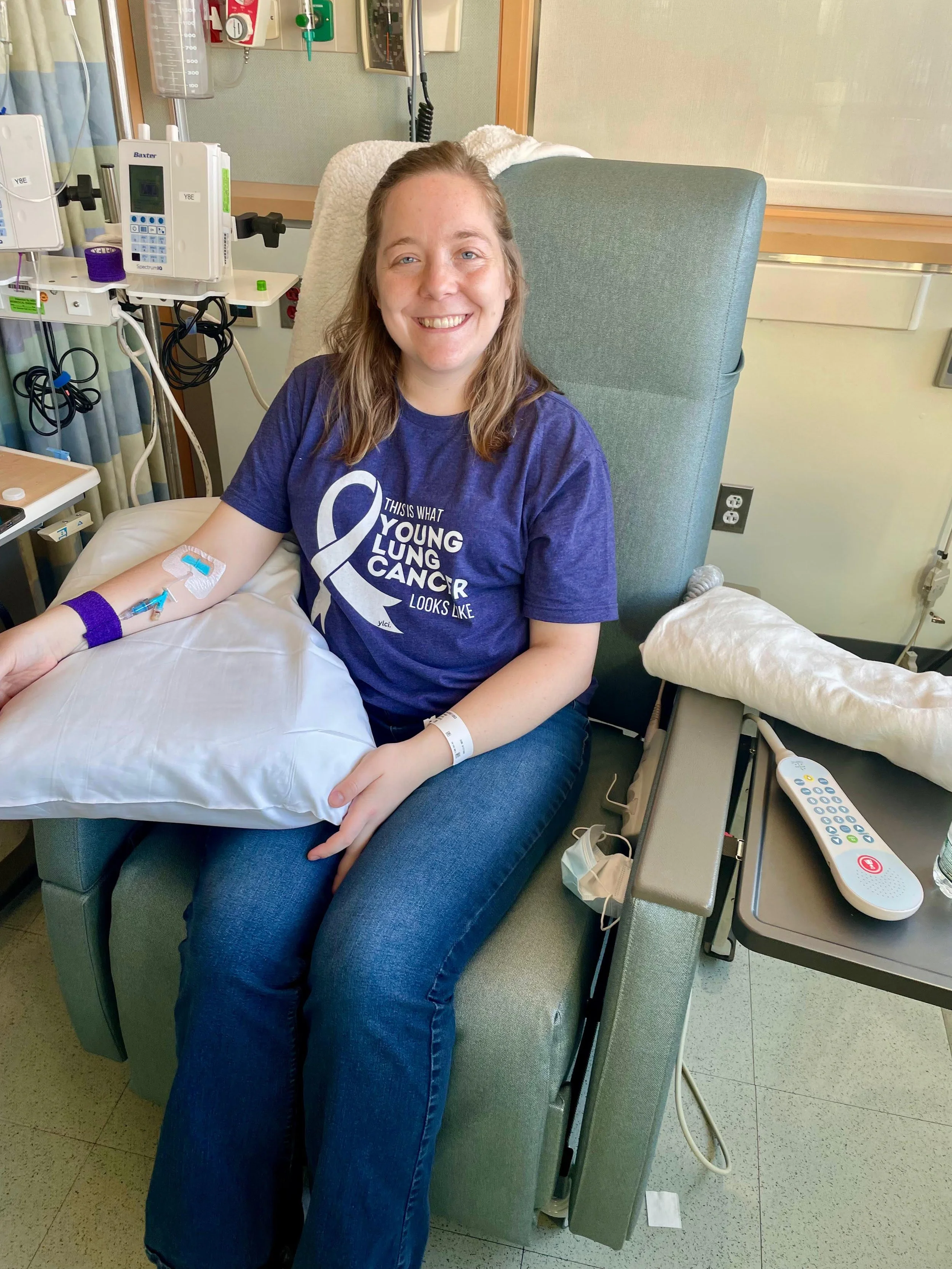
"I just imagined this meant that my cancer is much more aggressive. I feared that maybe the treatments just aren't going to work for me."
Then came Enhertu – the targeted therapy administered by infusion that is specifically for HER2-positive cancer.
Everything changed.
Loryn’s liver enzymes, which had spiked to 700 (normal is around 40), started dropping dramatically. The innumerable lesions in her liver began responding. Her bones started healing. She could walk again.
"I started getting some of my energy back," Loryn says. "The fatigue started going away. I started feeling more like myself again."
Loryn started swimming – something she began during radiation to regain strength without bearing weight. She still does it today, nearly a year into her Enhertu treatment.
"It helped me so much in the beginning," Loryn says. "I keep going because it reminds me of how far I've come.”
I started getting my energy back. I started feeling more like myself again.

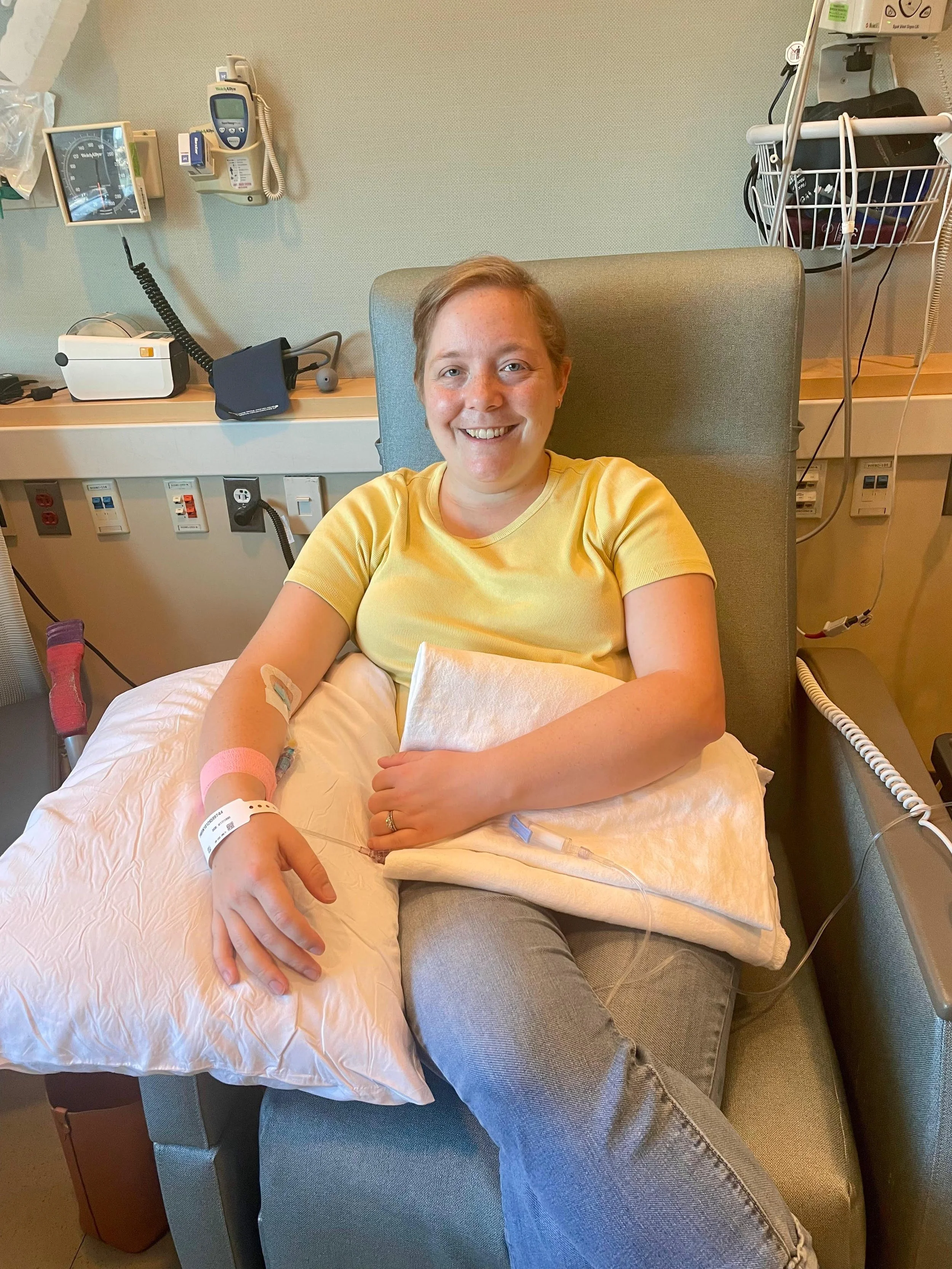
The new normal
Loryn is now 35. She goes to Boston every three weeks – sometimes every four now – for a two-hour infusion. The drive is two hours each way from Western Massachusetts.
She's lost her long, straight hair. It's growing back and a little curly now. She deals with fatigue and nausea, especially as the months on treatment accumulate. But she's stable. She's alive. And importantly, she's watching her son grow up.
Her life looks nothing like it did before cancer.
Loryn was working as a project manager, working 40-plus hours a week in a stressful job. When she was diagnosed, she went on family medical leave. She thought she'd go back. But her employer expected her to "hit the ground running again."
But Loryn knew she couldn't. She went on disability – a decision that still makes her feel guilty sometimes when she feels good.
"I have moments where I wonder if I should I be on disability," she admits. "But I think that program is there for a reason. I'm able to focus on my health now."
Her identity shifted. She went through what she calls "an identity crisis" – realizing how much of herself was tied up in her career. Her husband still works full-time. Her son still goes to school. Their lives continued mostly the same.

The power of being believed
Loryn credits her care team at Mass General with saving her life – not just medically, but emotionally.
"The first portion of our appointment is usually me venting about everything I'm dealing with," she says of her oncologist. "Then we get into the medicine. We have a very open relationship."
Her oncologist checks in with her whole life. Asks about her son. Connected them with a social worker who helped with heating bills and mortgage payments when money got tight. Provided gas cards for those long drives to Boston. Connected them with an oncology psychiatrist when her son started asking big questions about cancer.
Loryn has learned how to accept help. Friends take their son on chemo days so he doesn’t see his mother at her worst. Meals appear. Yard work gets done. Her husband’s firefighter community shows up in quiet, practical ways. Even now, more than a year later, neighbours still knock with food.

She also found her community – those from the Young Lung Cancer Initiative, other HER2-positive patients, people who understood what it was like to be young and facing the unexpected.
"My sister found a video of another HER2 lung cancer patient, pointing out that she was quite like me and suggesting we should connect," Loryn recalls. I just felt that by meeting others all the pieces started to fit together."
Seeing other young people with lung cancer living their lives gave Loryn something she desperately needed: hope.
She was also motivated to share her own story. “I didn’t choose this mutation,” she says. “But if having it means more research, more treatments, more people living longer — then I’ll talk about it. Loudly.”

Listen to your body
"I am really grateful for research," she says. "And while I've been on my drug, other treatments are popping up as options. We have an oral targeted therapy option available now. I have feel hopeful by seeing a focus now on HER2."
That hope – the research, the new treatments, the community – keeps her going.
Her advice to other patients echoes through every part of her story:
"Listen to your body and your intuition when things don't feel right. Even pre-diagnosis, I tried to just keep going. I didn't take what the doctors were telling me at face value. I felt that there had to be something more here. Even now, if something doesn't feel right, I message my team immediately."
She also emphasises finding the right care team – one that sees the whole person, not just the disease.
"Your intuition is really important. Finding the right care team is so important."

"For months I was being told that I had nothing," she says. "And I knew that there was something wrong with me. I did have that moment of relief – I was right, there was something wrong, and now we can treat it."
"But I was also really scared."
That fear hasn't left. Neither has the cancer. But neither has Loryn's determination to keep living, keep fighting, keep being present for every moment she can steal back from this disease.
Loryn is not cured. She lives with stage four lung cancer. But she is here. She is present. She is raising her son. She is building a life that holds both grief and gratitude at once.
And she is no longer invisible.
March 2025
